High antidepressant dose linked to self harm in youths
 When it comes to the link between
When it comes to the link between
antidepressants and suicidal behavior in
young people, dose may matter quite a
bit, a new study suggests.
The Food and Drug Administration has for
years required antidepressants to carry
warnings that they may increase the risk of
suicidal thinking and behavior in children
and adults under age 25. The study,
published online Monday by the journal
JAMA Internal Medicine, finds the risk for
deliberate self harm doubles when
depressed young people start treatment
with higher-than-usual doses.
The finding is one more reason for doctors
and families to carefully consider how and
whether to use the medications in young
people, researchers say.
"One can quibble about how much benefit
there is at typical doses, and my sense is
that the benefit is modest at best," says
the study's lead author, Matthew Miller, a
physician at the Harvard School of Public
Health. "But there's no evidence that
higher initial doses are going to help more
than lower doses." Instead, he says, higher
doses may only add risk.
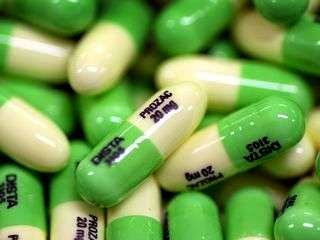
For the study, Miller and colleagues
looked at the health records of 162,625
privately insured people ages 10 to 64
treated for depression with three popular
antidepressants best known by the brand
names Celexa, Prozac and Zoloft.
They compared otherwise similar patients
— based on the intensity of their
depression symptoms, previous self harm
and other factors — who got either typical
starting doses or higher doses.
The typical starting doses were 20 mg. a
day for Celexa and Prozac and 50 mg. a
day for Zoloft.
Result: After a year, children, teens and
young adults were twice as likely to engage
in deliberate self harm if they started at
higher doses. Such acts were especially
common in the first three months. No
such link between starting dose and self
harm was found in adults 25 and up.
The number of young people who hurt
themselves was 142 out of 21,305. The
risk was 1.4% at typical doses and a 3.1%
at higher doses.
The reasons for any link between
antidepressants and self harm remain
unclear; it's also not known why it shows
up only in young people. One theory is
that the medications give young sufferers
new energy to carry out suicide plans;
another is that unpleasant side effects
trigger suicidal thoughts. Higher doses
might make such effects bigger, Miller and
his colleagues speculate.
The study adds support to guidelines that
call for starting antidepressants at low
doses, says David Brent, a professor of
psychiatry at the University of Pittsburgh
who co-wrote an accompanying editorial.
He notes that the study did not look at
whether dose escalations over time raised
risk.
Brent takes issue with Miller's statement
that antidepressants have "modest"
benefits in youths. For adults and youths
with depression of equal severity, he says,
benefits are comparable.
The National Institute of Mental Health
says the latest studies suggest "the benefits
of antidepressant medications likely
outweigh their risks to children and
adolescents with major depression." It
says that a combination of medication and
psychotherapy was most effective in one
major study.
The choices can be complex, Brent says:
"There is no one right thing to do. It's the
obligation of the physician to explain the
risks and benefits and for the family to
make the decision."
R. Scott Benson, a child psychiatrist in
Pensacola, Fla., says some children and
teens get put on antidepressants "in too
casual a way," without a thorough
evaluation of their problems. "We have to
make sure their level of depression is
serious enough to warrant treatment with
an antidepressant," he says. Benson is on
the communications committee of the
American Psychiatric Association.
Antidepressants are used by 3.7% of
children ages 12 to 17 and 6.1% of adults
ages 18 to 39, according to the federal
Centers for Disease Control and
Prevention. Use is higher in older adults.